January 25, 2010
The Vision Thing—For Real
By Michael D. Shaw
It is most interesting that the word “vision” refers both to the sense of sight, as well as to something perceived in a manner other than through one’s eyes. When presidential candidate George H.W. Bush asked a friend to help him identify some important issues for the upcoming campaign in 1988, it was suggested that Bush spend some time at Camp David to set his own presidential agenda.
Apparently unimpressed by his friend’s advice, Bush—long experienced with nitty gritty details, but sometimes lacking in gauging the big picture, or at least having difficulties in expressing it—sardonically replied, “Oh, the vision thing.”
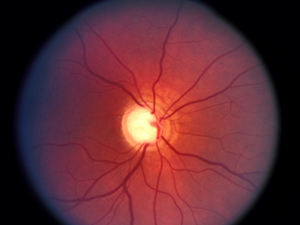
The big picture on glaucoma—the so-called “sneak thief of sight” since it has few early symptoms—is that this group of diseases represents the second leading cause of blindness (second only to diabetes). Vision loss derives from damage to the optic nerve, frequently identified with elevated intraocular pressure (IOP).
IOP is directly related to the amount of fluid (aqueous humor) within the eye, and can build up if the drainage system (trabecular meshwork) is not functioning properly.
While anyone can be at risk for glaucoma, some groups are more greatly affected:
- African Americans are five times more likely to contract glaucoma than Caucasians.
- In patients with glaucoma, African Americans are four times more likely to become blind than Caucasians, and between the ages of 45-64, this statistic jumps to 15 times more likely.
- While all people over the age of 60 are at greater risk, Mexican Americans seem to be hit especially hard.
- As in many conditions, family history can provide a risk factor.
Overall, glaucoma affects one in 200 people aged 50 and younger, and one in ten over the age of 80.
The Glaucoma Research Foundation points out that early detection, through regular and complete eye exams, is the key to protecting your vision from damage caused by glaucoma. Typical tests are tonometry, in which the IOP is measured, and ophthalmoscopy, whereby the interior of the eye—including the optic nerve—can be examined.
For those with the disease, typical treatment modalities involve medications such as eye drops or pills that act to lower the IOP, along with laser and conventional surgical intervention. Laser trabeculoplasty (remember that trabecular meshwork?) promotes better drainage. Conventional surgery creates actually creates a new opening for drainage. As with all drugs and surgical procedures, side effects and complications can occur. For some patients, compliance with the dosage schedule of the eye drops is a problem.
One novel therapy, called Pneumatic Trabeculoplasty (PNT), has been introduced by Ophthalmic International, a subsidiary of Sunridge International.
PNT is described by the company as a non-invasive, cost effective, alternative treatment for glaucoma and ocular hypertension, performed in the doctor’s office, under local (topical) anesthetic. PNT utilizes a vacuum fixation ring connected to a computerized vacuum controller. The ring is placed on the surface of the eye—held open by a speculum—and a vacuum is applied for one minute.
Five minutes later, the procedure is repeated; and this process can be reprised one week later, for even better results. IOP is checked one hour after the procedure. The duration of the IOP lowering effect is, on average, three to four months—at which time the procedure can be repeated. While PNT is approved in several countries outside of the United States (including Canada and the EEC), the product is under development here, and therefore is still considered an investigational device under current FDA regulations. Additional clinical trials are planned.
A number of recent studies attest to the safety and efficacy of PNT.
Approximately 75% of patients will exhibit an IOP reduction following PNT. Patients reported no serious side effects to vision and no changes in the visual field or optic nerve head. PNT can also be used for newly diagnosed patients who have yet to undergo pharmaceutical approaches.
Given the number of people affected by glaucoma, it is comforting that well over 100 clinical trials—implementing all sorts of therapies—are currently recruiting patients. For more information, visit NIH’s registry. The Glaucoma Research Foundation (GRF) also details advances in glaucoma treatment.
GRF recommends the following examination schedule:
- Before age 40, every two to four years
- From age 40 to age 54, every one to three years
- From age 55 to 64, every one to two years
- After age 65, every six to 12 months
- Anyone with high risk factors, every year or two after age 35

